Platelet-rich plasma (PRP) therapy is an increasingly popular chronic pain management treatment method.
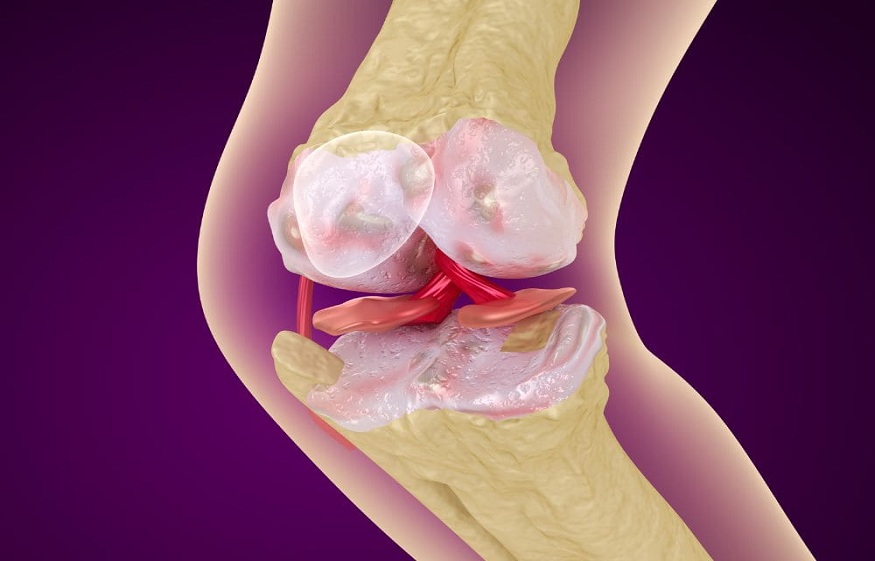
What Is Knee Osteoarthritis?
Osteoarthritis (OA) is a chronic joint disease that can affect people of all ages and is one of the most common chronic degenerative joint conditions.
OA affects the entire joint–bone, cartilage, fat, ligaments, and synovium, and it can:
- degrade cartilage
- change bone shape
- cause inflammation.
Knee osteoarthritis is divided into five stages:
- Stage 0 (Normal)
- Stage 1 (Minor)
- Stage 2 (Mild)
- Stage 3 (Moderate)
- Stage 4 (Severe).
Moderate knee OA shows clear cartilage damage and a narrowing of the space between your bones.
How Does PRP Therapy Work?
Platelet-rich plasma therapy is administered by pain management experts like the physicians and staff at Lone Star Pain Medicine in Weatherford, Texas.
PRP therapy works by collecting whole blood cells from a patient, extracting the PRP by separating the blood, then injecting the retrieved PRP in the affected area.
The effectiveness of PRP therapy lies in the presence of growth factors like thrombospondin-1 in the platelets, which are critical for joint repair. PRP also contains high levels of the other growth factors which support tissue regeneration.
PRP Therapy Contraindications
It’s essential that you discuss the potential risks and side-effects of PRP therapy with your primary care physician as the process should be avoided if one has been diagnosed with certain other conditions.
Also approach PRP therapy with caution if you take any of the following:
- anti-inflammatory medications
- systemic corticosteroid medications
- corticosteroid injection at the treatment site within 14 days before treatment.
PRP Retrieval, Preparation, And Injection
The basic steps are the same for most PRP therapy protocols:
- Whole blood is drawn, usually from your arm.
- The blood is placed in a centrifuge and separated into three layers of PRP, white blood cells (leukocytes), and red blood cells.
- The PRP is retrieved and injected into your knee.
If the leukocytes and red blood cells are discarded, you are left with leukocyte-poor PRP (LP-PRP). If the leukocytes – also known as the buffy coat – are incorporated, you have leukocyte-rich PRP (LR-PRP).
A study in Japan found that older patients undergoing LP-PRP therapy produced lower levels of platelet-derived growth factor-BB and insulin-like growth factor-1, making both LP-PRP and LR-PRP less effective in.
Effects of LP-PRP vs LR-PRP Therapy on Knee Osteoarthritis
Leukocytes or white blood cells produce fibroblast cells, which help maintain the structural integrity of connective tissue throughout the body.
Fibroblast cells are also essential in the synthesis of extracellular matrix proteins which support wound healing after an injury.
A 2020 study completed in Australia found that leucocyte-rich PRP enhances the properties and functions of fibroblasts in the healing process. However, the results of Stanford University study on LR-PRP point to “an early and acute inflammatory response compared with LP-PRP.”
Pain management doctors don’t yet know if such an acute pain response would speed up the healing process or prolong recovery since there is no indication of other adverse effects.
In the treatment of knee OA, LP-PRP was found to be more effective as it contained lower levels of interleukin-1β (IL-1β) and tumour necrosis factor-α that both increase inflammation and pain.
Final Thoughts
While more investigation is needed on the long-term inflammatory effects of leukocytes, platelet-rich plasma therapy has shown some promising results for knee OA and other forms of osteoarthritis.